Caveat Emptor: Foot placement is a complex thing.
/"Understanding why we place a foot where we do can be a choice, eventually a habit, of perceived stability, of compensation and we like to say "it is a sliding scale between liabilities and economy". If you want more running economy, go for a narrow step width, but realize you are wrestling with its underlying liabilities. The key is, one must have enough durability on the loading response of a narrow step width (cross over gait) to fend off the liabilities to reap the rewards of the improved economy. Forgo this principle, and it is caveat emptor."- Dr. Shawn Allen
Today we wanted to revisit a few topics and start to tie them together so that readers can perhaps more deeply bring the study discussed here today, into a deeper thought process.
We have discussed the topic of gluteal pain in chronic low back pain clients previously, when the 2015 Cooper article was published ahead of print. Well, it came out in print (Euro Spine J) in 2016 so we wanted to revisit it with some more global thoughts. Those links are below.
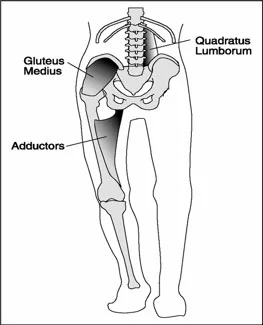
Basically, the article said that people with low back pain often have “Gluteus medius weakness and gluteal muscle tenderness are common symptoms in people with chronic non-specific LBP.”
As we mentioned in our blog post last year, commenting on the "ahead of print" article, "it is often more on the side of pelvic frontal plane drift. The abdominals and spinal stabilizers also often test weak on this same side. We often see compromise of hip rotation stability as well because , since the hip is relatively adducting (because the pelvis is undergoing repeated frontal plane drift, hence no hip abduction) there is often a component of cross over gait phenomenon which can threaten rotation stability of the lower limb (type “cross over gait” into the search box of our tumblr blog for a landslide of work we have written on that phenomenon)."
This brings to mind this brief (14minute excerpt) from an old podcast we did (#109b, link below) on foot targeting, pelvis frontal plane drift, glute weakness and cross over gait. We brought together several concepts in that 14 minute span and it was on the topic from the Rankin article (link below).
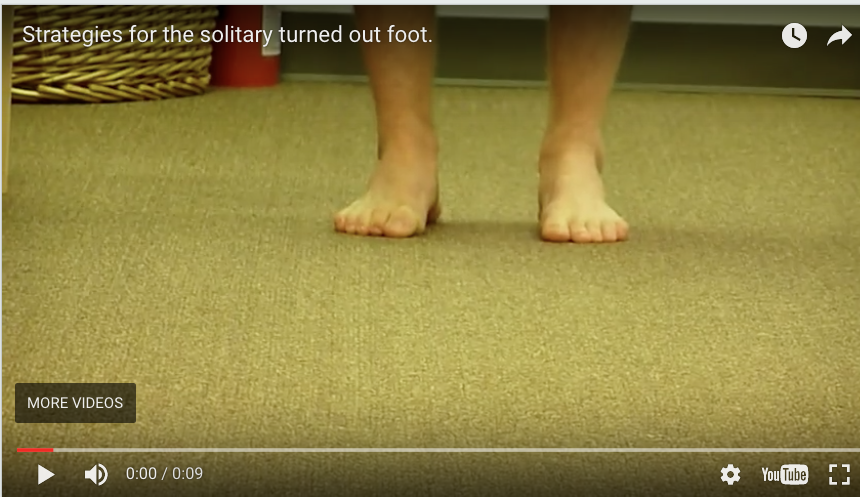
If one is treating clients one must put all these concepts together (one should also have a deep grasp of the principles in this video ). One cannot have tunnel vision, one must embrace the entire picture neuromechanically. Foot targeting, gluteus medius activity, frontal plane pelvis drift or sway, cross over gait parameters, limb torsional issues, foot types and many more must all come into play if you are to truly get to the bottom of your clients problems. The approach must look at the loading and movement patterns at the very least, from foot to pelvis. We would argue one should not stop there however, take your evaluation all the way into arm swing, thoracopelvic canister stability and more.
We have pounded sand on the cross over gait and arm swing and the like for almost a decade now. As far as we know, we introduced, and if not, at the very least were the ones that dove deep into the cross over gait and its issues, and all of the attributes and functional pathologic pieces that go with it. We feel that if you fully understand the 40+ articles we have written on the cross over gait and arm and leg swing you will take your client and athlete evaluation to another level. Understanding unconscious foot targeting is key in our opinion. "Understanding why we place a foot where we do can be a choice, eventually a habit, of perceived stability, of compensation and we like to say "it is a sliding scale between liabilities and economy". If you want more running economy, go for a narrow step width, but realize you are wrestling with its underlying liabilities. The key is, one must have enough durability on the loading response of a narrow step width (cross over gait) to fend off the liabilities to reap the rewards of the improved economy. Forgo this principle, and it is caveat emptor. "
Shawn & Ivo, the gait guys
https://thegaitguys.tumblr.com/post/149177564774/podcast-109b-shorts-the-gluteus-medius-during
A neuromechanical strategy for mediolateral foot placement in walking humans. Rankin BL
J Neurophysiol. 2014 Jul 15;112(2):374-83. doi: 10.1152/jn.00138.2014. Epub 2014 Apr 30.
Eur Spine J. 2016 Apr;25(4):1258-65. doi: 10.1007/s00586-015-4027-6. Epub 2015 May 26.
Prevalence of gluteus medius weakness in people with chronic low back pain compared to healthy controls.
Cooper NA1,2, Scavo KM3, Strickland KJ3, Tipayamongkol N3, Nicholson JD4, Bewyer DC4, Sluka KA3.
http://www.ncbi.nlm.nih.gov/pubmed/26006705