The Toe Waving Exercise: Part 1
Welcome to Friday, Folks. A little exercise here for you today that we use all the time.
There are at least 3 muscles important in forming and maintaining the foot tripod. The short flexors of the lesser digits (Flexor Digitorum Brevis or FDB) are one of the important component sfor creating and maintaining the foot tripod (the tripod between the head of the 1st metatarsal, head of 5th metatarsal and center of calcaneus).
It arises by a narrow tendon from the medial process of the calcaneal tuberosity the plantar aponeurosis, and from the connective tissue between it and the adjacent muscles. As it passes forward, and divides into four tendons, one for each of the four lesser toes which divide into 2 slips ( to allow the long flexor tendons to pass through), unite and divides a second time, inserting into the sides of the second phalanx.
Because the axes of the tendons passe anterior to the metatarsal phaalngeal joint (MTP), they also provide an upward (or dorsal) movement of the MTP joint complex, moving it posterior (or dorsal) with respect to the 1st metatarsal heal (thus functionally moving the 1st met head “down”). This is a boon for people with a forefoot varus, as it can help create more mobility of the 1st ray, as well as help descend the head of 1st ray to form the medial tripod (and assist the peroneus longus in anchoring the base of the big toe). It also helps the lumbricals to promote flexion of the toes at the MTP, rather than the distal interphalangeal joint.
In this brief video, Dr Ivo explains the exercise to a patient (Thank you N, for allowing us to use this footage).
The Toe Wave: try it. Use it with your patients. Spread the tripod. We know you want to….
Ivo and Shawn
all material copyright 2012: The Homunculus Group/The Gait Guys


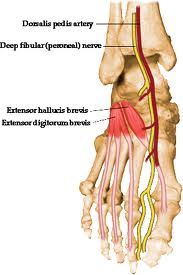 Did you know that the EHB (extensor hallucis brevis) the topic of today’s video tutorial, originates off of the forepart of the medial aspect of calcaneus & lateral talocalcaneal ligament. It is just above the bulk origin of the EDB (extensor digitorum brevis). It is frequently torn/strained in ankle inversion sprains and frequently goes undiagnosed. It can be torn/avulsed from the bone if the inversion sprain is focused below the lateral ankle joint. This occurs mostly when the foot is more plantarflexed before the inversion event. A foot cannot afford to have an impaired big toe ! Don’t miss this one !
Did you know that the EHB (extensor hallucis brevis) the topic of today’s video tutorial, originates off of the forepart of the medial aspect of calcaneus & lateral talocalcaneal ligament. It is just above the bulk origin of the EDB (extensor digitorum brevis). It is frequently torn/strained in ankle inversion sprains and frequently goes undiagnosed. It can be torn/avulsed from the bone if the inversion sprain is focused below the lateral ankle joint. This occurs mostly when the foot is more plantarflexed before the inversion event. A foot cannot afford to have an impaired big toe ! Don’t miss this one !

















