External tibial torsion and lower back pain
/How can external tibial torsion and lower back pain possibly be related? Let’s take a quick look at the anatomy and see how.
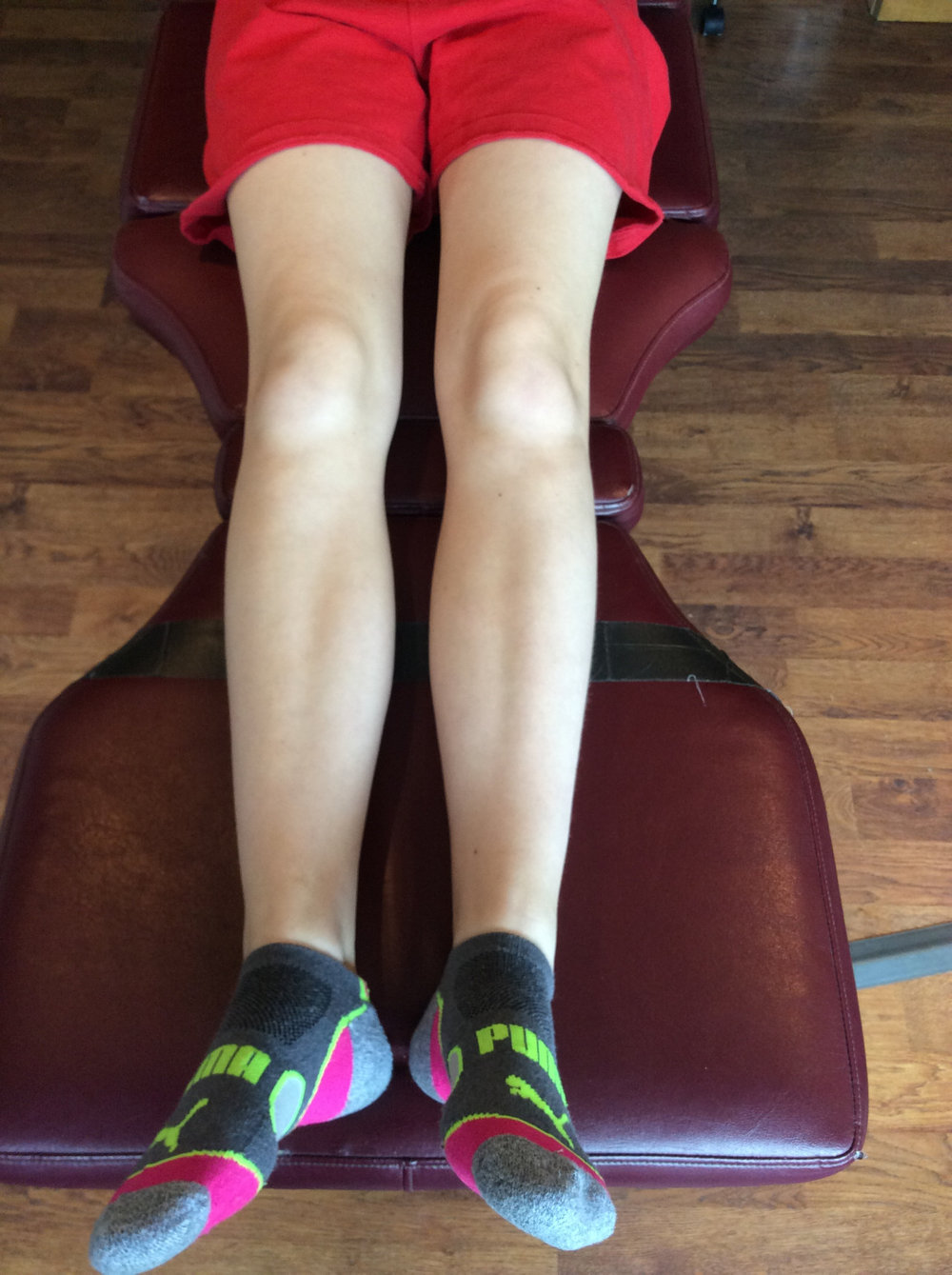
knees neutral, note external rotation of the right foot and decreased progression angle
Remember the external tibial torsion is present if we drop a plumbline from the tibial tuberosity and it passes between the first and second metatarsals or more medially. This increases the progression angle of the foot. This occurs due to “over rotation" of the lower extremity during development, often exceeding the 1.5 degrees per year of external rotation per year up to age 15 or occurring for a longer period of time, up to skeletal maturity. It can be uni or bilateral.
note when the foot is neutral, the knee points inward
Often, due to the increased progression angle, people will try to "straighten their feet" (ie, decrees their progression angle) to move forward in the sagittal plane. This places the knees to the inside of the sagittal plane which causes medial knee fall and sometimes increased mid and forefoot pronation. This results in increased medial spin of the thigh bilaterally which increases the lumbar lordosis. Combine this with a sway back or anterior pelvic tilt and you have increased pressure on the lumbar facet joints. The facets are designed to carry approximately 20% of the load put in these circumstances are often called upon to carry the much more. This often results in facet imbrication and lower back pain. You can strengthen the abdomen all you like but if you do not change the attitude of the foot, a will often develop lower back pain, especially when the abs fatigue. Now think about if the deformity is unilateral; this will often cause asymmetrical rotation of the pelvis in a clockwise or counter clockwise direction.
So, what can you do you?
Since external tibial torsion is a "hard deformity", we can influence how the bone grows before skeletal maturity but after that will not change significantly with stretching or exercise.
You can teach them to walk with an increase in progression angle (ie “duck footed”). This will often keep the knee in the sagittal plane and can be surprisingly well tolerated
You can use a foot leveling orthotic or arch support to bolster the arch and change the mechanics of the foot, causing external rotation of the tibia which will often result in a decrease in progression angle in compensation while still keeping the knee in the sagittal plane
You could place a full length varus wedge in the shoe which, by inverting the foot, externally rotates the tibia which the person will often compensates for by decreasing there progression angle to keep the knee and the sagittal plane
Dr Ivo Waerlop, one of The Gait Guys
#tibialtorsion #lowbackpain #LBP #progressionangle