1. Babst D, Steppacher SD, Ganz R, Siebenrock KA, Tannast M. The iliocapsularis muscle: an important stabilizer in the dysplastic hip. Clin Orthop Relat Res. 2011 Jun;469(6):1728-34. doi: 10.1007/s11999-010-1705-x. Epub 2010 Dec 3.link to full text: http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3094621/
2. Anatomy of the iliocapsularis muscle. Relevance to surgery of the hip.Ward WT, Fleisch ID, Ganz R Clin Orthop Relat Res. 2000 May; (374):278-85.
3. HOLLINSHEAD W. H. (ed), Anatomy for surgeons: the back and limbs, vol. 3, Harper & Row, New York, 1969, 707.
4. SUJATHA D’COSTA, LAKSHMI A. RAMANATHAN, SAMPATH MADHYASTHA, S. R. NAYAK, LATHA V. PRABHU, RAJALAKSHMI RAI, VASUDHA V. SARALAYA, PRAKASH An accessory iliacus muscle: a case report Romanian Journal of Morphology and Embryology 2008, 49(3):407–409 link to full text : http://www.rjme.ro/RJME/resources/files/490308407409.pdf
5. Retchford TH1, Crossley KM, Grimaldi A, Kemp JL, Cowan SM Can local muscles augment stability in the hip? A narrative literature review. J Musculoskelet Neuronal Interact. 2013 Mar;13(1):1-12. link to full text: http://www.ismni.org/jmni/pdf/51/01RETCHFORD.pdf
6. Lawrenson P, Grimaldi A, Crossley K, Hodges P, Vicenzino B, Semciw AI. Iliocapsularis: Technical application of fine-wire electromyography, and direction specific action during maximum voluntary isometric contractions. Clin Orthop Relat Res. 2015 Dec;473(12):3725-34. doi: 10.1007/s11999-015-4382-y.
7. Haefeli PC, Steppacher SD, Babst D, Siebenrock KA, Tannast M. An increased iliocapsularis-to-rectus-femoris ratio is suggestive for instability in borderline hips. Clin Anat. 2015 Jul;28(5):665-71. doi: 10.1002/ca.22539. Epub 2015 Apr 14.
8. Walters BL, Cooper JH, Rodriguez JA. New findings in hip capsular anatomy: dimensions of capsular thickness and pericapsular contributions. J Musculoskelet Neuronal Interact. 2013 Mar;13(1):1-12.
9. Cooper HJ, Walters BL, Rodriguez JA1.Anatomy of the hip capsule and pericapsular structures: A cadaveric study. Arthroscopy. 2014 Oct;30(10):1235-45. doi: 10.1016/j.arthro.2014.05.012. Epub 2014 Jul 23.
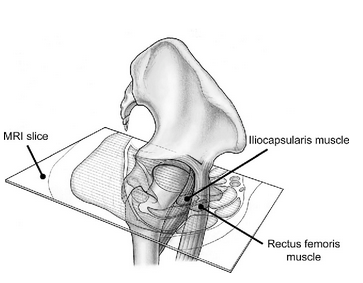
image credit: Haefeli, Pascal Cyrill et al. “An increased iliocapsularis-to-rectus-femoris ratio is suggestive for instability in borderline hips.” Clinical orthopaedics and related research 473 12 (2015): 3725-34.