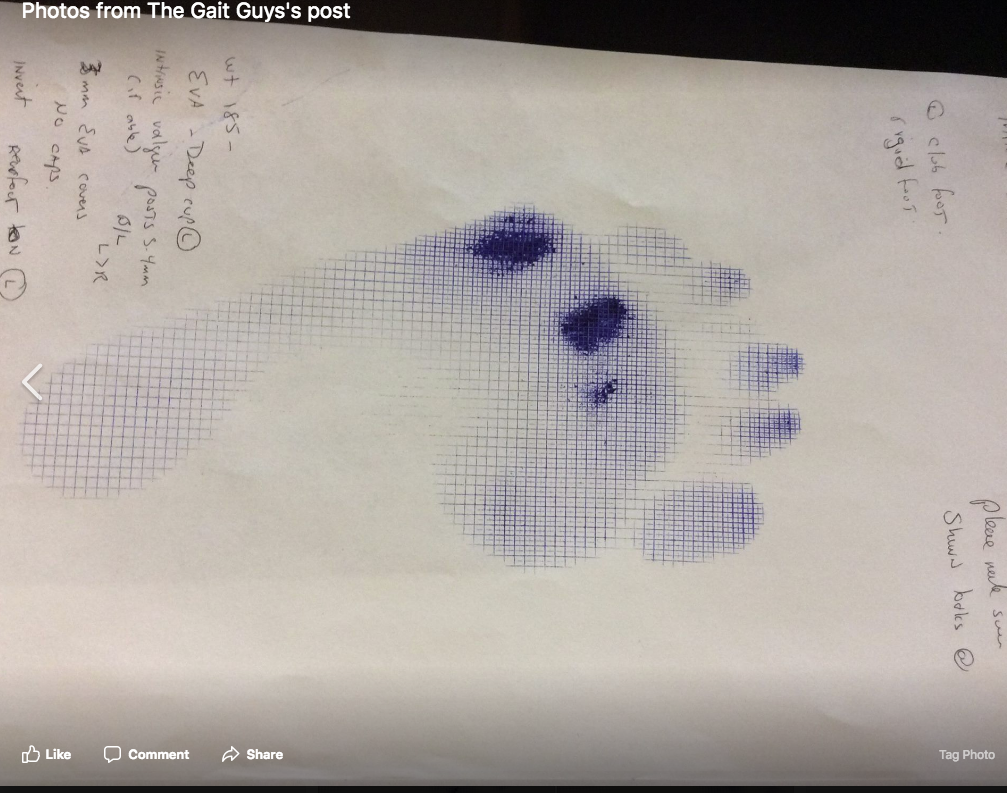
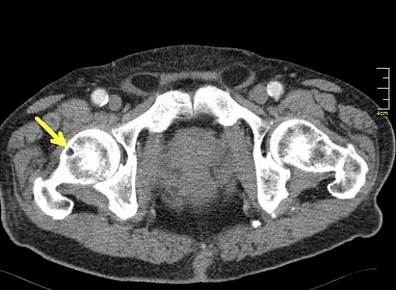
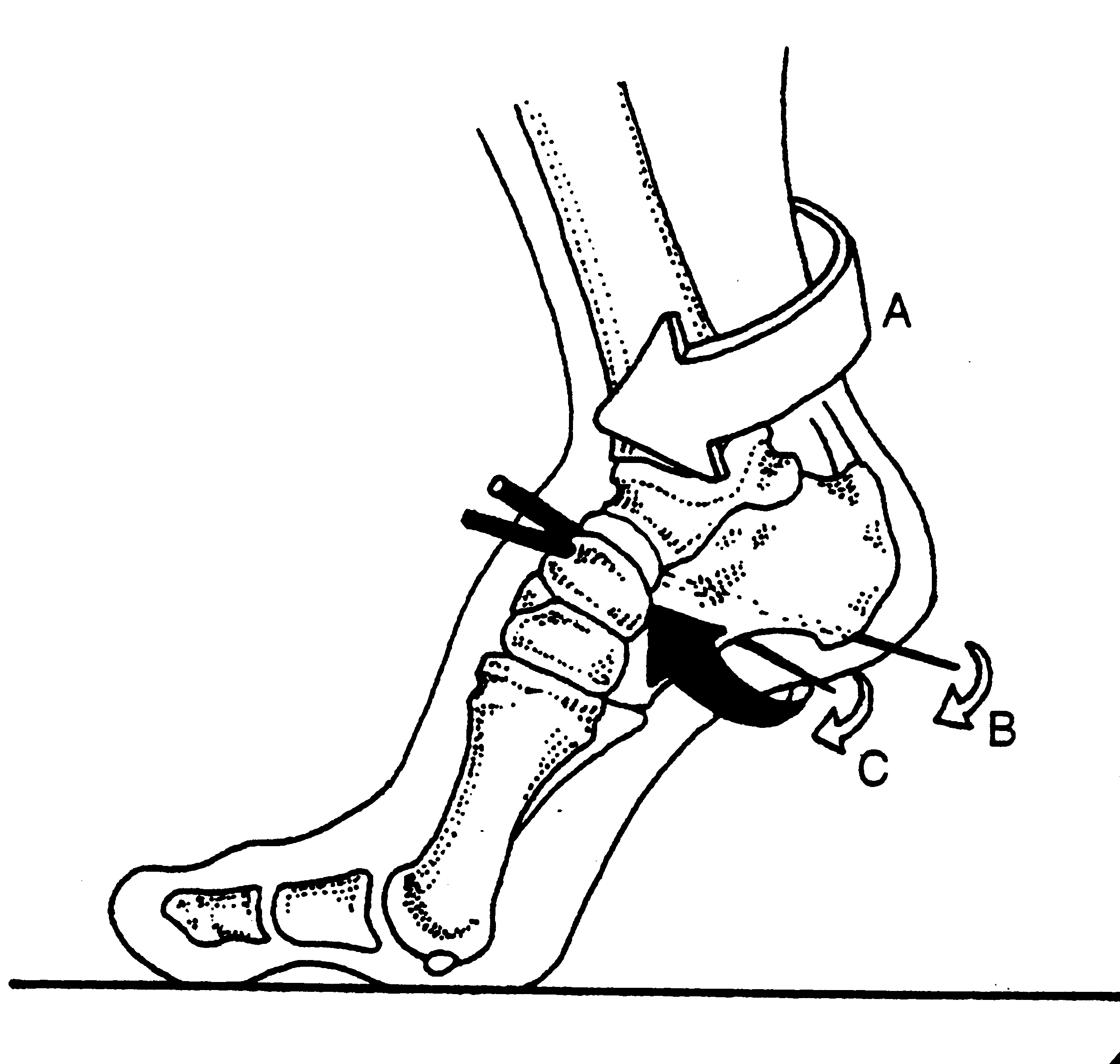
Key Tag Words: thegaitguys, gait, gait analysis, hallux rigidus, hallux limitus, calf strength, calf endurance
Links to find the podcast:
http://traffic.libsyn.com/thegaitguys/pod_131f.mp3
http://thegaitguys.libsyn.com/podcast-131
iTunes page: https://itunes.apple.com/us/podcast/the-gait-guys-podcast/id559864138?mt=2
http://directory.libsyn.com/episode/index/id/5958375
Our Websites:
www.thegaitguys.com
summitchiroandrehab.com doctorallen.co shawnallen.net
Our website is all you need to remember. Everything you want, need and wish for is right there on the site.
Interested in our stuff ? Want to buy some of our lectures or our National Shoe Fit program? Click here (thegaitguys.com or thegaitguys.tumblr.com) and you will come to our websites. In the tabs, you will find tabs for STORE, SEMINARS, BOOK etc. We also lecture every 3rd Wednesday of the month on onlineCE.com. We have an extensive catalogued library of our courses there, you can take them any time for a nominal fee (~$20).
Our podcast is on iTunes, Soundcloud, and just about every other podcast harbor site, just google "the gait guys podcast", you will find us.
Show Notes:
Researchers turn skin cells into motor neurons without using stem cells
https://futurism.com/researchers-turn-skin-cells-into-motor-neurons-without-using-stem-cells/
Immune cells release “red flag” to activate muscle stem cells in response to damage
http://scopeblog.stanford.edu/2017/09/25/immune-cells-release-red-flag-to-activate-muscle-stem-cells-in-response-to-damage/
Does structural leg-length discrepancy affect postural control? Preliminary study.
Eliks M, et al. BMC Musculoskelet Disord. 2017.
Evidence for Joint Moment Asymmetry in Healthy Populations during Gait. Rebecca L. Lambach et al. Gait Posture. 2014 Sep; 40(4): 526–531.
J Phys Ther Sci. 2017 Jun; 29(6): 1001–1005.
Published online 2017 Jun 7. doi: 10.1589/jpts.29.1001
PMCID: PMC5468184
Does the weakening of intrinsic foot muscles cause the decrease of medial longitudinal arch height?
Kazunori Okamura, RPT, MS,1,* Shusaku Kanai, RPT, PhD,2 Sadaaki Oki, MD, PhD,2 Satoshi Tanaka, RPT, PhD,2 Naohisa Hirata, RPT, MS,3 Yoshiaki Sakamura, RPT, MS,4 Norikatsu Idemoto, RPT,1 Hiroki Wada, RPT,1 and Akira Otsuka, RPT, PhD5