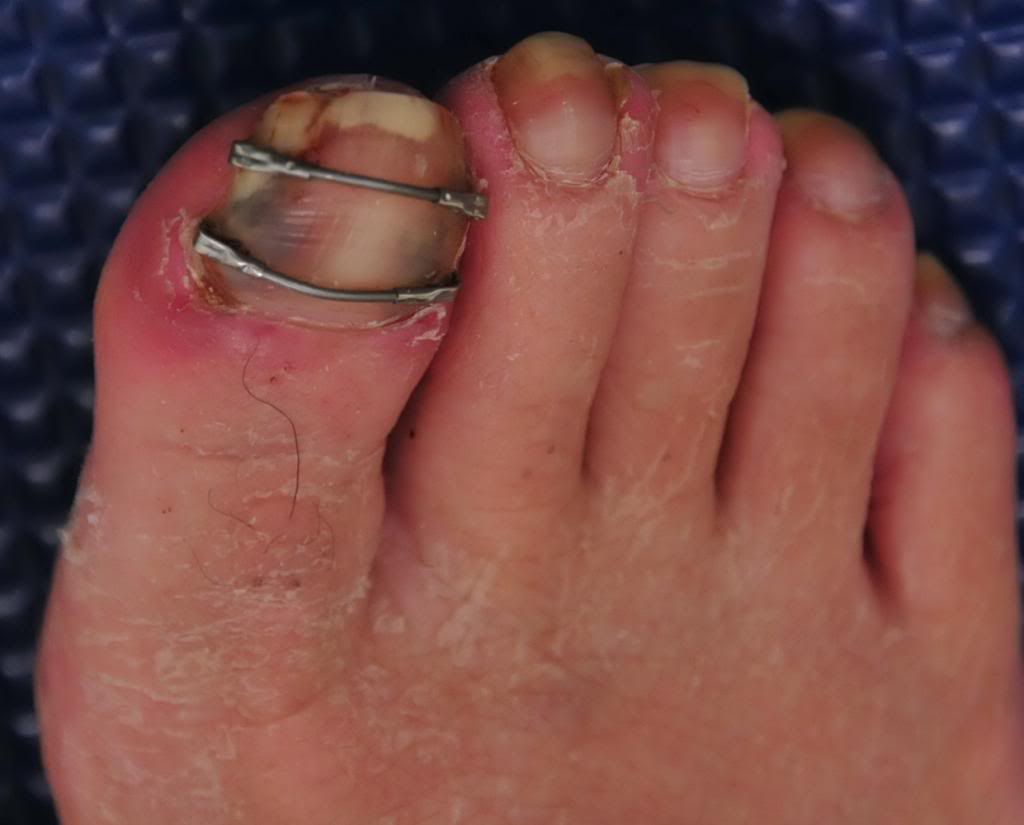
Pincher nails. Who knew !?
Written by Dr. Shawn Allen
*note: there are two photos here in today’s blog post, look for the side scroll arrows and click on the small box in the upper left corner if you cannot see the photo
We have seen this one for years in our clinics but we never got around to researching it and pondering the condition more deeply. Here is our mantra for today, Form follows Function.
Studies seem to be undecided on the cause of this entity. Some suggest that pincer nails are caused by lack of upward mechanical forces on the toe pad where others remark that they can be observed amongst the healthy mechanical walkers. Hitomi’s study suggests that the affected toes fail to receive adequate physical stimulation from proper toe and forefoot loading. Please read on, this gets interesting.
According to Hitomi’s study, in both the barefoot and shod state,
“the pincer nail group had significantly lower pressure on the first toe than the control group. In both the barefoot and shod state, the peak pressure area was mostly the metatarsal head area in the pincer nail group, whereas it was mostly the first toe area in the control group. Binomial logistic regression analysis revealed that peak pressure area was a significant risk factor for pincer nail development.”
This seems to suggest that there is insufficient or aberrant use of downward pressure on the toes and into the toe pads. Hitomi speaks of the locale of the peak pressure, seemingly proposing from this study that it should not be under the metatarsal heads. This, in our experience and thinking, could suggest that more long flexor dominance is present. This long flexor activity seems to create some disfunction not only in the activity of the lumbrical muscles but also altered pressures in the metatarsal (MET) heads. It certainly alters distal toe pressures which can alter skin and nail responses (see our blog post on subungal hematomas for more on this topic where we discuss principles of counter pressure and shear forces). We try to teach a “spread and reach with long flat toes” approach to our clients in correcting bad habits such as toe hammering and gripping (which are often a result of flawed biomechanics elsewhere).
The nail bed is very rich in vasculature (hence the cause of the dreaded hematoma, the black toenail) and nerve endings. The nail bed is a derivative of the epidermis containing keratin which gives it its hard nature. The nail consists of the nail plate, the nail fold, the nail matrix, the sterile matrix and the hyponychium. There are many factors that go into the formation of a normal nail, including blood flow, nutrition, local neurogenic factors and not to forget, mechanical loading issues. Failure of any of these issues can lead to softening, brittle, thinning, diseased or malformed nails. The nail grows from a nail root in front of the cuticle and grows distally at a slow but (usually) steady rate. It is interesting to note that the long extensor tendon (EDL) attachment is close to the proximal nail bed root area thus it brings forward thinking of possible imbalances between long and short flexors and extensor tendons/muscles and their patterns of imbalance in toe gripping and hammering that could cause a change in function which could drive a change in form. We have all heard it, form follows function, why should this area be any different ?
Hitomi also mentioned something interesting in his study, the observation that bed ridden clients seem to have a predilection to pincer toes. This at least seems to fit the aberrant loading patterns, in this case an absence of. The study also started some interesting thinking in us when it mentioned a hypothesis,
“that human nails are constitutively equipped with an automatic shrinkage function that allows them to adapt to daily upward mechanical forces.”
This was a fascinating hypothesis to us. It seems to make sense. If constant downward pressure on the toe pads were present, the toe nails would always be undergoing a flattening and spreading response so it could make sense that the nails have a built in curve and shrinkage function offsetting and adapting to the constant distorting pressures (the flattening and spreading forces). Hence, some possible clarity in Hitomi’s hypothesis that pincer nails are caused by lack of (and in our thinking, distorted) upward mechanical forces on the toe pad. And, when those distorting pressures are placed elsewhere (ie. the MET heads or tips of the toes as in our subungal hematoma hypothesis) or faulting gripping or hammering loading the automatic shrinkage function is left to dominate.
We think Hitomi’s hypothesis is correct. Here is why (this is paraphrased from our blog post on subungal hematomas and our revolutionary thinking on why they occur and it seems to fit well with pincer nail formation as well).
… when the skin is pulled at a differential rate over the distal phalange (from gripping of the toes rather than downward pressing through the toe pad) there will be a net lifting response of the nail from its bed as the skin is drawn forward of the backward drawn phalange (there is a NET movement of skin forward thus lifting the nail from its bedding). For an at-home example of this, put your hand AND fingers flat on a table top. Now activate JUST your distal long finger flexors so that only the tip of the fingers are in contact with the table top (there will be a small lifting of the fingers). There should be minimal flexion of the distal fingers at this point. Note the spreading and flattening of the nail. Now, without letting the finger tip-skin contact point move at all from the table, go ahead and increase your long flexor tone/pull fairly aggressively. You are in essence trying to pull the finger backward into flexion while leaving the skin pad in the same place on the table. Feel the pressure building under the distal tip of the finger nail as the skin is RELATIVELY drawn forward.] This is fat pad and skin being drawn forward (relative to the phalange bone being drawn backward) into the apex of the nail. Could this be magnifying the curvature of the nail and not offsetting the “automatic curving and shrinkage” function of the nail ? We think it is quite possible.
So, there you have it. We will dive deeper on this topic another time, but after reading Hitomi’s study our brain’s started buzzing because we had discussed this process similarly a few years back in our Subungal Hematoma blog post.
And, if you are thinking about chronic repeated ingrown toe nails with this clinical entity, your thoughts are clearly on a logical path. There is a correlation it seems.
And, as for the horrific metal bar correction you see in the other photo above, this too is new to our eyes. It seems rather medieval, something one might see in the gallows of yesteryear. And if that doesn’t curl your hair and make you nauseated, try looking at what this one guy did, a DIY remedy (caution, not for the feint of heart). https://www.mja.com.au/journal/2005/182/4/diy-pincer-nail-repair-brace-yourself
ShawnAllen, one of the gait guys
References:
Foot loading is different in people with and without pincer nails: a case control study Hitomi Sano1*, Kaori Shionoya2 and Rei Ogawa1 Journal of Foot and Ankle Research 2015, 8:43